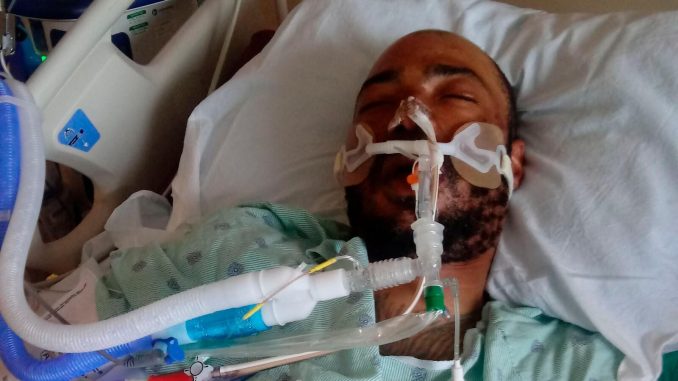
Demetrio Jackson was desperate for medical help when the paramedics arrived.
The 43-year-old was surrounded by police who arrested him after responding to a trespassing call in a Wisconsin parking lot. Officers had shocked him with a Taser and pinned him as he pleaded that he couldn’t breathe. Now he sat on the ground with hands cuffed behind his back and took in oxygen through a mask.
Then, officers moved Jackson to his side so a medic could inject him with a potent knockout drug.
“It’s just going to calm you down,” an officer assured Jackson. Within minutes, Jackson’s heart stopped. He never regained consciousness and died two weeks later.
Jackson’s 2021 death illustrates an often-hidden way fatal U.S. police encounters end: not with the firing of an officer’s gun but with the silent use of a medical syringe.
The practice of giving sedatives to people detained by police has spread quietly across the nation over the last 15 years, built on questionable science and backed by police-aligned experts, an investigation led by The Associated Press has found. Based on thousands of pages of law enforcement and medical records and videos of dozens of incidents, the investigation shows how a strategy intended to reduce violence and save lives has resulted in some avoidable deaths.
At least 94 people died after they were given sedatives and restrained by police from 2012 through 2021, according to findings by the AP in collaboration with FRONTLINE (PBS) and the Howard Centers for Investigative Journalism. That’s nearly 10% of the more than 1,000 deaths identified during the investigation of people subdued by police in ways that are not supposed to be fatal. About half of the 94 who died were Black, including Jackson.
Behind the racial disparity is a disputed medical condition called excited delirium, which fueled the rise of sedation outside hospitals. Critics say its purported symptoms, including “superhuman strength” and high pain tolerance, play into racist stereotypes about Black people and lead to biased decisions about who needs sedation.
The use of sedatives in half these incidents has never been reported, as scrutiny typically focuses on the actions of police, not medics. Elijah McClain’s 2019 death in Aurora, Colorado, was a rare exception: Two paramedics were convicted of giving McClain an overdose of ketamine, the same drug given to Jackson. One was sentenced last month to five years in prison and the other was sentenced Friday to 14 months in jail and probation.
It was impossible to determine the role sedatives may have played in each of the 94 deaths, which often involved the use of other potentially dangerous force on people who had taken drugs or consumed alcohol. Medical experts told the AP their impact could be negligible in people who were already dying; the final straw that triggered heart or breathing failure in the medically distressed; or the main cause of death when given in the wrong circumstances or mishandled.
While sedatives were mentioned as a cause or contributing factor in a dozen official death rulings, authorities often didn’t even investigate whether injections were appropriate. Medical officials have traditionally viewed them as mostly benign treatments. Now some say they may be playing a bigger role than previously understood and deserve more scrutiny.
Time and time again, the AP found, agitated people who were held by police facedown, often handcuffed and with officers pushing on their backs, struggled to breathe and tried to get free. Citing combativeness, paramedics administered sedatives, further slowing their breathing. Cardiac and respiratory arrest often occurred within minutes.
Paramedics drugged some people who were not a threat to themselves or others, violating treatment guidelines. Medics often didn’t know whether other drugs or alcohol were in people’s systems, although some combinations cause serious side effects.
Police officers sometimes improperly encouraged paramedics to give shots to suspects they were detaining.
Responders occasionally joked about the medications’ power to knock their subjects out. “Night, night” is heard on videos before deaths in California, Tennessee and Florida.
Emergency medical workers, “if they aren’t careful, can simply become an extension of the police’s handcuffs, of their weapons, of their nightsticks,” said Claire Zagorski, a former paramedic and an addiction researcher at the University of Texas at Austin.
Supporters say sedatives enable rapid treatment for drug-related behavioral emergencies and psychotic episodes, protect front-line responders from violence and are safely administered thousands of times annually to get people with life-threatening conditions to hospitals. Critics say forced sedation should be strictly limited or banned, arguing the medications, given without consent, are too risky to be administered during police encounters.
Ohio State University professor Dr. Mark DeBard was an important early proponent of sedation, believing it could be used in rare cases when officers encountered extremely agitated people who needed rapid medical treatment. Today, he said he’s frustrated officers still sometimes use excessive force instead of treating those incidents as medical emergencies. He’s also surprised paramedics have given unnecessary injections by overdiagnosing excited delirium.
Others say the premise was flawed, with sedatives and police restraint creating a dangerous mix. The deaths have left a trail of grieving relatives from coast to coast.
“They’re running around on the streets administering these heavy-duty medications that could be lethal,” said Honey Gutzalenko, a nurse whose husband died after he was injected with midazolam in 2021 while restrained by police near San Francisco. “It’s just not right.”
Jackson was standing on a truck outside a radio station on the border of the small Wisconsin cities of Eau Claire and Altoona. An employee called 911 before dawn on Oct. 8, 2021, hoping officers could shoo away a stranger who “doesn’t seem to be a threat, but not normal either.”
Police video and hundreds of pages of law enforcement and medical records show how the incident escalated.
An Altoona police officer met Jackson in the parking lot. Jackson appeared uneasy and paranoid, looking around and talking softly. He had taken methamphetamine, which a psychiatrist said he used to self-medicate for schizophrenia. He’d been in and out of jail and living on the streets, with frequent visits to the emergency room seeking a place to rest.
The officer, joined by a second Altoona officer and a sheriff’s deputy, told him he could leave if he gave his name. Jackson refused.
Police identified him through his tattoos, learning he was on probation for meth possession. They noticed the truck had minor damage and decided to arrest him.
Jackson took off running. The officers chased Jackson, who stopped seconds later and staggered toward the first officer. Body-camera video shows she fired her Taser, its darts striking Jackson in the stomach and thigh. He screamed after the electrical shock and collapsed.
When officers couldn’t handcuff Jackson, she fired additional darts, striking Jackson in the back as he lay on the ground. Officers from the Eau Claire Police Department forced Jackson onto his stomach to be handcuffed and restrained him in what’s known as the prone position.
“I’m begging you to stop,” Jackson said. “I can’t breathe.”
After a couple of minutes, officers moved him to his side and then sat him up, trying to improve his breathing.
An officer wondered aloud whether Jackson had “excited delirium” and asked a colleague if paramedics were “going to stand around and do nothing.” He voiced approval when one arrived with ketamine, adding Jackson would not like it “when he gets poked.”
The Eau Claire Fire Department’s excited delirium protocol advises, “Rapid sedation is the key to de-escalation!!!!!” The medic measured 400 milligrams after estimating the 6-foot-tall Jackson weighed 175 pounds, enough to immobilize someone within minutes. He injected the medicine into Jackson’s buttocks.
Five medical experts who reviewed the case for AP said Jackson’s behavior did not appear to be dangerous enough to justify the intervention.
“I don’t believe he was a candidate for ketamine,” said Connecticut paramedic Peter Canning, who said he supports sedating truly violent patients because they stop fighting and are sleeping by the time they get to the hospital.
Minutes later, Jackson stopped breathing on the way to Sacred Heart Hospital. He’d suffered cardiac arrest and, after he was resuscitated, had no brain function.
Jackson’s mother, Rita Gowens, collapsed while shopping at an Indiana Walmart when she learned her oldest son was hospitalized and not expected to survive.
Gowens rushed to the hospital 500 miles away, where she was told he’d been injected with ketamine. She searched online and was stunned to read it’s used to tranquilize horses.
Gowens spoke to Jackson, held his hand and hoped for a miracle. She eventually agreed to remove him from a ventilator after his condition didn’t improve, singing into his ear as he took his final breaths: “You’ve never lost a battle, and I know, I know, you never will.”
She still has nightmares about how police and medics treated her son, whom she recalls as a happy boy with chunky cheeks that inspired the nickname “Meatball.” There are few days when she doesn’t ask, “Why did they give him an animal tranquilizer?”
The practice of using ketamine to subdue people outside hospitals began in 2004 when a disturbed man scaled a fence, cut himself with a broken bottle and paced along a narrow strip of concrete on a Minneapolis highway bridge.
The man was in danger of falling into traffic below when officers reached through the fence and grabbed him.
Dr. John Hick, who worked with first responders, heard the emergency radio chatter while driving and rushed to the scene with an idea. Hick gave the man two shots of ketamine, started an IV and kept him breathing with an air mask.
The man stopped struggling, and responders lowered him to safety.
Paramedics had occasionally used other sedatives to calm combative people since the 1980s. Hick and his Hennepin County Medical Center colleague Dr. Jeffrey Ho believed ketamine worked faster and had fewer side effects, showing promise to avert fatal police encounters.
Ho was a leading researcher on Taser safety and an expert witness for the company in wrongful death lawsuits. In a 2007 deposition in one such case, he argued for a potentially “life-saving tactic” of having sedative injections quickly follow Taser shocks, saying the combination could shorten struggles that, if prolonged, might end in death.
Some doctors at his public hospital in Minneapolis were using “something called ketamine, which is an analog to LSD,” he said. “It’s sort of an animal tranquilizer.”
The drug became more common outside the hospital in 2008 when Hennepin County paramedics were given permission to use it.
An American College of Emergency Physicians panel that included Ho said in 2009 that ketamine had shown “excellent results and safety” while acknowledging no research proved it would save lives.
In time, its use became standard from Las Vegas to Columbus, Ohio, to Palm Beach County, Florida. The earliest death involving ketamine documented in AP’s investigation came in 2015, when 34-year-old Juan Carrizales was injected after struggling with police in the Dallas suburb of Garland, Texas.
Shortly after ketamine became authorized for such use in Arizona in 2017, deputies who were restraining David Cutler facedown in handcuffs in the scorching desert asked a paramedic to sedate him.
The medic testified he was surprised when Cutler stopped breathing, although the dose was larger than recommended for someone weighing 132 pounds. He said he had been trained that ketamine didn’t impact respiration. Cutler’s death was ruled an accident due to heat exposure and LSD — though that was disputed by experts hired by Cutler’s family, who said heat stroke along with ketamine caused his death.
In Minneapolis, an oversight agency found the use of ketamine during police calls rose dramatically from 2012 through 2017 and body-camera video showed instances of officers appearing to pressure paramedics to use ketamine and joking about its power. The department told officers they could never “suggest or demand” the use of sedation.
Facing criticism, Hennepin Healthcare halted a study examining the effectiveness of ketamine on agitated patients. The Food and Drug Administration later found the research failed to protect vulnerable, intoxicated people who had not given consent.
By 2021, the American College of Emergency Physicians warned ketamine impacted breathing and the heart more than previously believed.
“Ketamine is not as benign as we might have hoped it to be,” a co-author of the new position, Dr. Jeffrey Goodloe, said on the group’s podcast in 2022.
He said the practice of giving large doses of ketamine, sometimes too much for smaller patients, had spread nationwide as agencies copied each other’s protocols with little independent review.
But the AP’s findings show risks of sedation go beyond ketamine, which was used in at least 19 cases.
Roughly half of the 94 deaths documented by the AP came after the use of midazolam, which has long been known to heighten the risk of respiratory depression. Many came during police encounters in California, where ketamine is not widely used. Midazolam, a common pre-surgery drug known by the brand name Versed, is also part of a three-drug cocktail used in some states to execute prisoners.
Other cases involved a range of other drugs, including the antipsychotic medications haloperidol and ziprasidone, which can cause irregular heartbeats.
The need for monitoring side effects is often laid out for paramedics in written guidelines, many of which are based on the disputed belief that excited delirium can cause sudden death.
The theory of excited delirium was troubling from the start.
In the 1980s, with cocaine use soaring, Dr. Charles Wetli, a Miami forensic pathologist, coined the term to explain a handful of deaths of violent cocaine users, many of whom had been restrained by police. Wetli, who died in 2020, also blamed excited delirium for the mysterious deaths of more than a dozen Black women. He said cocaine and sexual activity triggered the fatal condition.
The women’s deaths eventually were attributed to a serial killer. Wetli’s theory survived. And over time, symptoms described by Wetli and others — “superhuman strength,” animal-like noises and high pain tolerance — became disproportionately assigned to Black people. The terms spread to police and emergency medical services to describe certain agitated people — and explain sudden deaths.
By the mid-2000s, police were encountering more drug users and mentally ill people as stimulant use increased and psychiatric hospitals closed. Departments adopted Tasers as a less-lethal alternative to firearms, but there was a problem — hundreds died after being jolted.
Supporters of Wetli’s research, including the medical examiner in Miami-Dade County, ruled again and again that excited delirium was the cause of these deaths, not the effects of the weapons and other physical force. Executives at Taser’s manufacturer agreed, promoting excited delirium to medical examiners around the country and retaining experts who explained the concept to juries in wrongful death lawsuits.
In 2006, a grand jury that investigated Taser-related deaths in Miami-Dade recommended an untested treatment that it said could save people before they died from excited delirium: squirting midazolam up their noses to cause “almost immediate sedation.” Its report acknowledged they “may experience difficulty in breathing.” Miami-Dade paramedics adopted this treatment.
But key medical groups didn’t recognize excited delirium, and activists were calling for limits on Taser use. What happened next would help promote sedation alongside Tasers as tools to gain control.
In 2008, the biggest names in excited delirium research gathered at a Las Vegas hotel for a three-day meeting organized by a group with ties to Taser’s manufacturer.
“A lot of talk took place on chemical sedation because the cops didn’t know what to do with these people,” recalled John Peters, president of the Institute for the Prevention of In-Custody Deaths, which sponsored the meeting. “Jeff Ho had done some work up in Minnesota. He said, ‘Look. I’ve been using ketamine. It knocks them out quicker.’”
The timing was fortuitous: The American College of Emergency Physicians would soon form a task force to study excited delirium and how police and medics should respond.
The 19-member panel included Ho, who became Taser’s medical director under an arrangement in which the company paid part of his hospital salary; Dr. Donald Dawes, a Taser research consultant; and University of Miami researcher Deborah Mash, who testified for Taser about several deaths she blamed on excited delirium. At least two other panelists were routinely retained by officers and their departments as expert witnesses.
The panel’s 2009 paper disclosed none of these relationships. It found excited delirium was real, could result in death regardless of whether someone was shocked with a Taser and called for “aggressive chemical sedation” to treat the symptoms.
DeBard, the now-retired Ohio doctor who chaired the panel, told AP he recruited relevant experts to join and that disclosure of conflicts wasn’t required by the ER doctors group then. He said Taser didn’t influence the outcome, which reflected the panel’s consensus. Mash said she had no conflict because Taser didn’t fund her research. Dawes declined an interview request. Ho didn’t return messages.
Taser rebranded itself in 2017 as Axon. A spokesperson for the company declined interview requests and did not respond to written questions.
Dr. Brooks Walsh, an emergency physician in Connecticut who was not on the panel, said the 2009 paper reinforced racial bias as it formalized “loaded terms” used to describe excited delirium, influencing how the diagnosis would be applied.
Ho and other Taser- and police-aligned experts joined a federally sponsored panel in 2011 that built on the work, recommending four actions on a checklist for officers and paramedics: Identify excited delirium symptoms; control (with a Taser if necessary); sedate; and transport to a hospital.
No test measures for excited delirium, so paramedics faced a judgment call: Which patients were so agitated, strong, impervious to pain and dangerous that they needed to be sedated?
DeBard said the symptoms were based on medical observations, not race. “If you’ve got somebody that’s delirious, irrational, aggressive, hyperactive, running around naked, I mean, it’s really pretty easy” to recognize, he said.
Yet, over time, prominent medical groups and some experts pointed to overuse of sedation during police encounters and a disproportionate impact on Black people. Even supporters of the practice have acknowledged that the wrong patients at times have been injected.
The deaths of Black men in police custody, including the 2020 killing of George Floyd, put pressure on the medical community to re-examine excited delirium. The ER doctors group in 2023 withdrew approval of the 2009 paper and said excited delirium shouldn’t be used in court testimony. Some doctors called that decision political and note the group still recognizes a similar condition — hyperactive delirium with severe agitation — that can be treated with sedation. But today no major medical association legitimizes excited delirium.
In more than a dozen cases reviewed by AP, police asked for or suggested the use of sedatives, calling into question whether medics were working for law enforcement or in patients’ interests. Officers often suggested their detainees had excited delirium.
University of California, Berkeley, law and bioethics professor Osagie Obasogie, who has studied excited delirium and sedation, said officers should be banned from influencing medical care.
“We need to be sure that folks are treated in a way that meets their medical needs and not simply given a chemical restraint because it’s convenient for law enforcement,” he said.
Officers are told not to dictate medical treatment but “some knuckleheads” have done otherwise, said Peters, whose group hosted the 2008 Las Vegas meeting that focused on excited delirium.
Paramedics say they make medical decisions independently from police, following guidelines that call for sedating people who may be dangerous. But in several cases AP found, people were injected though they had calmed down or even passed out after struggles with police.
Ivan Gutzalenko, a 47-year-old father, was struggling to breathe as two officers restrained him in Richmond, California. Gutzalenko told the officers they were hurting him, and bucked to try to get one off his back.
A paramedic viewed Gutzalenko’s action as aggression, and went to his ambulance to get a 5-milligram dose of midazolam. When he returned three minutes later, Gutzalenko lay motionless. “He’s faking like he’s unconscious,” an officer said.
The medic plunged the needle into his bicep. Gutzalenko’s heart stopped. He was declared dead at a hospital. A pathologist testified that midazolam was given to “quiet him down” during an episode of excited delirium but did not contribute to the death, which he blamed on prone restraint and meth use.
His wife said Gutzalenko, a former critical care nurse, would never have consented to receive midazolam that day.
“I know from being a registered nurse since 2004, you don’t administer a sedative to someone who is clearly already in respiratory distress,” she said, adding that his death has been devastating to their two teenage children.
Dr. Gail Van Norman, a University of Washington professor of anesthesiology and pain medicine, said it’s dangerous for officers to put pressure on the backs and necks of detainees before and after they’re injected with sedatives.
“It’s a recipe for disaster, because you may have created a situation in which you are impeding a person’s ability to get oxygen,” she said.
The AP investigation found half who died following sedation had been shocked with a Taser and the majority had been restrained facedown.
Their blood acid levels may already have been spiking from drugs, adrenaline and pain while oxygen levels may have been plummeting — life-threatening conditions called acidosis and hypoxia.
Sedatives can dull the instinct to compensate by breathing quickly and heavily to blow off carbon dioxide, essential for the heart to beat, said Dr. Christopher Stephens, a UTHealth Houston anesthesiologist and former paramedic.
Under sedation, he said, the body doesn’t respond as efficiently to the buildup of carbon dioxide. “Your brain doesn’t care as much about it,” Stephens said. “And they can go into respiratory and cardiac arrest.”
Paramedics usually have no idea whether their patients have alcohol, opioids or other depressants in their bodies that increase sedatives’ effects on breathing.
More than a dozen who died had been drinking, including Jerica LaCour, 29, a Colorado Springs, Colorado, mother of five young children.
She was stressed about family finances, husband Anthony LaCour recalled, when deputies found her trespassing at a trucking company.
“Guess who gets ketamine?” paramedic Jason Poulson of AMR, the nation’s largest ambulance company, said as LaCour was restrained on a gurney, according to body-camera footage.
An EMT said in a report that she told Poulson that LaCour had calmed and didn’t need ketamine, and later warned that LaCour was no longer breathing. In a disciplinary agreement with state regulators, Poulson admitted he was unsuccessful in protecting LaCour’s airway despite multiple attempts, mishandled the syringe and failed to document the ketamine use properly. His state certification was put on probation.
AMR and Poulson denied responsibility for LaCour’s death in court filings, arguing LaCour was experiencing excited delirium and ketamine was appropriate. This week they settled a long-pending wrongful death lawsuit, LaCour family attorney Daniel Kay said Friday. He said the settlement amount was confidential and the proceeds would help her children. AMR didn’t immediately respond to a request for comment and a man who answered a cellphone number listed for Poulson hung up on a reporter.
When people died, the use of sedation often went unacknowledged publicly and unquestioned by investigators.
After Jackson’s death in Wisconsin, police press releases said nothing about ketamine. State police redacted mention of the drug from investigation records and blurred video of the prone restraint and injection, saying his family’s privacy outweighed the public interest in disclosure.
The fire department, which declined comment, blacked out the information in its incident report. But when AP uploaded the document, redactions disappeared, revealing Jackson was given 400 milligrams of ketamine.
An autopsy concluded Jackson died from complications caused by meth. The report said Jackson’s ketamine dose was 100 milligrams, a quarter of what the fire department report said.
Two longtime forensic pathologists who reviewed the case for AP said meth use wasn’t the only factor. Dr. Joye Carter said she believed the police altercation and ketamine caused the death, saying the sedative can cause heart problems when given to a meth user.
Dr. Victor Weedn said the level of meth in Jackson’s blood was high but generally not lethal. He said Jackson likely died from high blood acid levels, with police restraint and possibly ketamine contributing.
The autopsy was performed in Ramsey County, Minnesota. A county spokesperson defended the findings from a now-retired medical examiner, saying the discrepancy on the ketamine dose wasn’t significant.
Citing the autopsy’s finding that meth was the cause, Eau Claire County District Attorney Peter Rindal ruled Jackson’s case was not an “officer-involved death” under Wisconsin law and closed the investigation.
In nearly 90% of the deaths examined by AP, coroners and medical examiners did not list sedation as a cause or contributing factor. Some autopsy reports failed to document that the deceased had been sedated.
The most common ruling was an accidental death in which other drugs, often meth or cocaine, were causes or contributing factors. More than a quarter were at least partially attributed to excited delirium.
Medical examiners view sedatives as safe treatments to control patients and wouldn’t question their use unless there was a grievous error, said Dr. James Gill, the chief medical examiner of Connecticut and past president of the National Association of Medical Examiners.
“Generally we’re going to default then back to what’s the underlying disease or injury that started this chain of events,” Gill said.
He said sedatives rarely cause deaths by themselves but additional studies could look at whether they play a role in fatal police struggles where many factors are involved.
Even when autopsies implicated sedatives, investigations didn’t always follow.
In LaCour’s case, the coroner found she died from “respiratory arrest associated with acute alcohol and ketamine intoxication.” The district attorney’s office said it had no record of reviewing her death.
Nine miles from LaCour’s injection, a paramedic injected 26-year-old Hunter Barr with ketamine as officers held him facedown in the dirt outside his Colorado Springs home in September 2020.
Retired postal worker Mark Barr had called 911 for help controlling his son, who he said wasn’t violent but was having a bad reaction to LSD. He watched as a medic gave two injections just minutes apart. He said he couldn’t figure out why the second injection was necessary, saying his son was subdued. Hunter Barr became unconscious on the way to a hospital and died within hours.
The coroner ruled Barr died from the effects of ketamine. The Colorado Springs Police Department closed the case as “non-criminal” and the DA’s office again had no review.
When deaths were investigated, inquiries usually focused on whether police used excessive force. In audio and video reviewed by AP, investigators seemed uninterested in how sedation may have contributed.
“I’m not trying to get in the weeds with a whole bunch of that,” an investigator told a paramedic explaining the ketamine injection he gave 18-year-old Giovani Berne before Berne’s heart stopped in Palm Bay, Florida, in 2016.
Berne’s sister, Christina, said the family didn’t know he had been given ketamine until contacted by AP years later, but “we knew something bad happened in the ambulance.” A medical examiner ruled that Berne died of excited delirium.
The death of McClain, 23, in Colorado is the only one that resulted in charges against paramedics. Prosecutors argued Aurora paramedics Jeremy Cooper and Peter Cichuniec didn’t assess McClain, gave him too much ketamine for someone his size and didn’t monitor him afterward.
Their convictions shook the EMS field, whose leaders say treatment mistakes shouldn’t be criminalized. Defense attorneys argued the paramedics followed their training on excited delirium and ketamine. A judge gave Cichuniec five years in prison while Cooper was sentenced Friday to 14 months in jail and probation.
Civil liability is also rare, in part because deaths have multiple causes and some courts have ruled that unwilling injections aren’t excessive force even when they cause harm. That hasn’t stopped families from trying: A number of wrongful death lawsuits involving sedation are pending.
Lawmakers in Colorado banned excited delirium as a justification for using ketamine and put other restrictions on the drug, but changes in the law elsewhere have been few.
Paramedic reformers are working to address the failures that increase the risk of sedatives contributing to deaths.
Paramedic Eric Jaeger helped rewrite New Hampshire’s protocols and, at a fire station in Hooksett, recently used Jackson’s death as a training scenario after evaluating the case for AP. He questioned whether sedation was necessary. He said medics failed to thoroughly evaluate Jackson and should have had monitoring equipment ready before any injection.
He said he had been aware of a handful of deaths but the number found by AP “dramatically increases” the scope.
“If we don’t change the training, change the protocols, change the leadership to make the system safer,” Jaeger said, “then we all bear responsibility for future deaths.”
___
Associated Press researcher Rhonda Shafner contributed from New York.
___
The Associated Press receives support from the Public Welfare Foundation for reporting focused on criminal justice. This story also was supported by Columbia University’s Ira A. Lipman Center for Journalism and Civil and Human Rights in conjunction with Arnold Ventures. Also, the AP Health and Science Department receives support from the Howard Hughes Medical Institute’s Science and Educational Media Group. The AP is solely responsible for all content.
___
Contact AP’s global investigative team at Investigative@ap.org or https://www.ap.org/tips/
___ This story is part of an ongoing investigation led by The Associated Press in collaboration with the Howard Center for Investigative Journalism programs and FRONTLINE (PBS). The investigation includes the Lethal Restraint interactive story, database and the documentary, “Documenting Police Use Of Force,” premiering April 30 on PBS.
—-
This story has been corrected to reflect that Claire Zagorski is a former paramedic instead of a paramedic


Be the first to comment